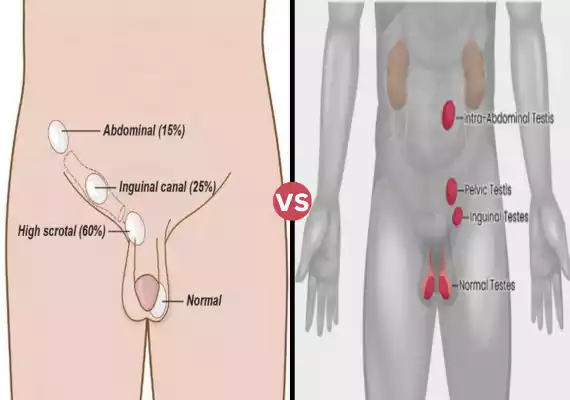
Undescended Testis and Retractile Testis are two testicular conditions, one often requiring surgery, and the other usually not, characterized by differences in testicle positioning
Undescended Testis: This is when a boy’s testicle doesn’t drop down into his scrotum like it should. It usually happens in babies and can sometimes fix itself, but if it doesn’t, a doctor might need to move it into the right place with surgery to avoid future problems with fertility and cancer.
Retractile Testis: A retractile testis is a normal condition where a testicle can move up and down in the scrotum. It can sometimes look like it’s not in the right place, but it can easily be pushed down by hand and is not a big concern. Unlike an undescended testis, a retractile testis doesn’t usually need surgery or special treatment.
What is Undescended Testis?
An undescended testis, also known as cryptorchidism, is a condition where a boy’s testicle doesn’t move down into the scrotum as it should during fetal development. Instead, it remains up in the abdomen or in the groin. This condition can occur in one or both testicles.
Undescended testes are more common in premature babies, but they can affect full-term babies too. It’s important to address this issue because the testicles need to be in the scrotum for proper development and to work effectively.
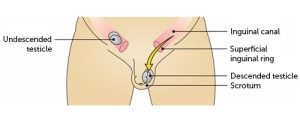
If left untreated, undescended testes can lead to problems with fertility and an increased risk of testicular cancer. Treatment often involves a surgical procedure called orchiopexy, which moves the testicle into the scrotum.
It’s crucial to address undescended testes in early childhood to ensure normal testicular development and reduce the risk of future health issues. Regular check-ups with a healthcare provider are essential to monitor and manage this condition.
What is Retractile Testis?
A retractile testis is a condition where a boy’s testicle can move up and down within the scrotum, but it’s not a cause for major concern. Unlike an undescended testis, a retractile testis typically starts in the scrotum during fetal development.
It can later move up into the groin area or higher in the scrotum, especially in response to cold or fear. This movement can sometimes make it seem like the testicle is not in the right place, but it’s usually temporary.

The good news is that a retractile testis can usually be easily pushed back down into the scrotum. It doesn’t usually require surgery or special treatment, and it doesn’t lead to fertility problems or an increased risk of cancer.
In most cases, it’s a normal variation, and healthcare providers will simply monitor it to ensure it doesn’t cause any issues as the child grows.
Difference Between Undescended Testis and Retractile Testis
Here’s a comparison chart between Undescended Testis and Retractile Testis:
| Aspect | Undescended Testis | Retractile Testis |
|---|---|---|
| Definition | The testicle doesn’t descend into the scrotum as it should during development. | The testicle can move up and down inside the scrotum, often in response to external factors like cold or fear. |
| Age Occurrence | Common in infants and young children. | Can occur in childhood but is less common. Typically seen in early childhood and not as common in adults. |
| Need for Surgery | Often requires surgical correction (Orchiopexy). | Surgery is usually not needed. |
| Reason for Surgery | To improve future fertility and lower the risk of testicular cancer. | Generally not recommended as it’s a normal variation and doesn’t usually lead to health concerns. |
| Fertility Concerns | May lead to fertility issues if left untreated. | Typically doesn’t lead to fertility problems. |
| Cancer Risk | Slightly increased risk of testicular cancer if not treated. | Not associated with an increased risk of testicular cancer. |
| Management | Requires medical intervention and monitoring. | Focuses on observation and education. |
What is the Main Cause of Undescended Testis or Cryptorchidism?
The main cause of cryptorchidism, also known as undescended testis, is not fully understood, but it likely involves a combination of genetic, hormonal, and environmental factors. Some common contributing factors include:
- Premature Birth: Babies born prematurely are more likely to have undescended testes because the testicles may not have had enough time to descend into the scrotum during fetal development.
- Hormonal Imbalances: Hormones play a crucial role in the descent of the testicles. Disruptions in the hormonal signals that guide the testicles into the scrotum can lead to cryptorchidism.
- Genetic Factors: There is evidence to suggest that there may be a genetic component to cryptorchidism, meaning it can run in families.
- Maternal Risk Factors: Some factors during pregnancy, such as maternal smoking or exposure to certain environmental toxins, may increase the risk of a baby being born with undescended testes.
- Low Birth Weight: Low birth weight is associated with an increased risk of cryptorchidism.
Can an undescended testicle occur at age 30?
Although testicular lesions that are not descended (cryptorchidism) are typically recognized and treated during the early years, it is still possible for this condition to be found or remain in adulthood, even after the age of 30 or more. Here are some key information:
- Uncommon in adulthood: Undescended testicles are typically treated in infants or in childhood. As adults, the majority of testicles have regressed into the scrotum either naturally or after treatment. There are instances in which this issue is not recognized or treated earlier in life.
- Potential Problems: An undescended testicle in adulthood may still present a risk. It can alter fertility by decreasing the production of sperm as well as increasing the chance of developing testicular cancer within the testicle.
- Medical Examination: If you suspect or have been diagnosed with an unscented testicle at the age of adulthood It is essential to speak with your doctor or another healthcare professional. They’ll conduct an extensive assessment, possibly including a physical examination, ultrasound as well as hormone testing.
- Solutions for Treatment: Treatment for undescended testicles in adulthood usually requires surgical procedures similar to those used for orchiopexy performed in children. The objective is to shift the testicle to the scrotum, which will increase fertility and lower the risk of developing cancer.
- Timing is Important: Timely treatment is crucial to increase the likelihood of a successful outcome, especially in relation to the preservation of fertility and reducing the risk of cancer.
What is the Main cause of Retractile Testis?
The primary cause of a retractile testis is the natural mobility of the testicle within the scrotum. This mobility is often triggered by external factors like cold or fear. Unlike an undescended testis, a retractile testis is not a result of a permanent problem or anatomical abnormality.
It’s usually a normal variation in testicular positioning. The testicle can move up and down, but it doesn’t stay permanently in an abnormal place. There is typically no underlying medical condition or known cause for this, and it does not usually lead to health concerns, making it a benign and naturally occurring condition.
Retractile Testicle in Adults
In adults, a retractile testicle is when one or both testicles can move up and down inside the scrotum. This can happen when it’s cold or you’re stressed, and it’s usually not a problem.
It’s less common in adults than in children, and it doesn’t typically lead to health issues. If you notice it, it’s a good idea to see a doctor to make sure everything is okay, but in most cases, it’s a normal and harmless thing.000
Clinical Tests and Diagnosis
- Physical Examining: The doctor will examine the scrotum and groin to find the testicles. If the testis is not descendent it is possible that the testicle may be absent from the scrotum.
- Ultrasound: It is a simple test that makes use of sound waves to make images. It assists the doctor to locate the testicle and determine the health condition.
- Hormone Tests: Sometimes blood tests are conducted to determine the level of hormones in order to better understand the problem.
- Note: For retractile tests, the possibility is that there won’t be any tests. Doctors will be watching it for a while to ensure it’s not creating issues.
- Medical history: A doctor can ask about birth records and also if there’s a family history of these conditions.
Treatment of Undescended Testis and Retractile Testis
Undescended Testis:
- Orchiopexy: It is surgery through which the undescended testicle is removed from its original place (abdomen or groin) into the scrotum. The surgeon creates a small incision to locate the testicle and then secures it to the scrotum with sutures. This procedure is usually done when the child is a few months old, to boost fertility in the future and reduce the chance of developing cancer of the testicle.
- Laparoscopy: In certain instances, when the testicle can’t be found in the groin area Laparoscopic surgery might be required. It is the use of a tiny camera and instruments to locate it and then relocate the testicle.
- Hormone Therapy: For certain scenarios hormone treatments can be considered in order to boost the process of descent of the testicle. Surgery is typically the preferred and most effective treatment.
Retractile Testis:
- Monitoring: Doctors will keep an eye on the condition throughout regular check-ups to make sure the testicle is mobile and does not cause problems.
- education: Healthcare providers and parents must educate the patient about the retractile testis, in order to ease concerns and avoid any unnecessary manipulation or intervention.
- Non-Surgical: Unlike undescended testes the retractile tests do not typically require surgery or other specific treatments.
When and why is Surgery needed for Undescended and Retractile Testes?
Surgery is sometimes required in the case of retractile and undescended tests the reasons for this and timeframes differ for each type of condition.
Undescended Testis: The surgery, also known as orchiopexy, is generally suggested. It is usually done when a child is about a month old, to reposition the testicle out of the abdomen, or even the groin area into the scrotum.
The main motives behind this procedure are to increase fertility in the future and decrease the risk of cancerous testicular tissue. Testes that are not ascending tend to not yield healthy sperm, and they are at greater risk of developing cancer if they are placed in the wrong location.
Retractile Testis: Surgery is typically not required for retractile tests. The condition involves an ovary that moves inside the scrotum, usually when it is in response to fear or cold it is not a problem.
The main focus is being aware and educating yourself to stay clear of unnecessary interventions. Surgery is not generally advised for tests of retractability since it’s an inherent variation and does not usually cause health issues.
A consultation with a physician is vital to figure out the best method of treatment for these ailments depending on the individual’s age and the particular characteristics of the tests.
Summary
Undescended Testis is when a boy’s testicle doesn’t properly move into the scrotum, often necessitating surgical treatment to prevent future fertility issues and lower the risk of cancer. A Retractile Testis refers to a testicle that can move within the scrotum, often in response to external factors like cold or fear.
This is typically a normal variation and rarely requires surgery, with medical observation sufficing to ensure it doesn’t lead to problems as the child grows. Retractile Testis doesn’t usually cause fertility or cancer concerns.