Streptococcus pneumoniae and Diplococcus Pneumoniae
Streptococcus Pneumoniae and Diplococcus Pneumoniae is that Streptococcus pneumonia exists as cocci chains and Diplococcus pneumonia exists in pairs of cocci.
Streptococcus pneumoniae, commonly referred to as pneumococcus, is a Gram-positive bacteria responsible for various respiratory and invasive infections. Distinguished by oval-shaped lancet-like cocci arranged in chains.
This bacteria has become one of the primary contributors to pneumonia, otitis media, sinusitis, meningitis, and bacteremia particularly problematic among children, elderly persons, and individuals with compromised immune systems. Pneumococcal infections represent a global health concern.
On the other hand, there is no known bacteria called “Diplococcus pneumoniae.” Instead, “diplococcus” refers to a shape seen in certain bacteria where two cocci are arranged side by side – such as Neisseria species (such as Neisseria gonorrhoeae and Neisseria meningitides) with similar arrangements.
But they’re usually not associated with pneumonia; if you think you have seen one mislabeled as “diplococcus pneumoniae,” they likely mislabeled or misidentified; for any specific bacterium related to pneumonia Streptococcus pneumoniae is likely your best choice as its name implies.
Definition of Streptococcus Pneumoniae
Streptococcus pneumoniae, more commonly referred to as pneumococcus, is an infectious species responsible for an array of human infections. Its properties include being Gram-positive, oval-shaped, and lancet-like coccus bacteria with chain-forming capabilities.
When observed under the microscope this strain is one of the primary causes of pneumonia, sinusitis, and otitis media infections in vulnerable populations such as young children, the elderly, or those with compromised immune systems.
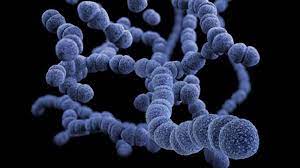
Streptococcus pneumoniae stands out from its peers due to its unique polysaccharide capsule that surrounds each cell and serves as a vital virulence factor, protecting it from host immune responses while increasing disease outbreaks.
Pneumococcal infections range in severity from mild respiratory tract infections to life-threatening invasive diseases like meningitis and bacteremia, placing public health at great risk.
Due to this threat, pneumococcal vaccines have been created as protection against some of the most prevalent serotypes of Streptococcus pneumoniae and thus reduce both the incidence and severity of pneumococcal diseases.
Effective diagnosis, antibiotic treatment with appropriate medications, and vaccination programs have played critical roles in managing and preventing Streptococcus pneumoniae infections that impact global health.
Definition of Diplococcus Pneumoniae
Diplococcus pneumonia is a gram-positive bacterium that is responsible for the development of pneumonia. Diplococcus is an elongated bacterium that typically appears in the form of two cells joined. D.
Pneumoniae is a bacterium that needs catalase in order to thrive on agar plates. These bacteria are typically recognized because they’re catalase-negative and sensitive to optochin. undergo lysis through alpha-hemolysis and bile salts in blood agar.
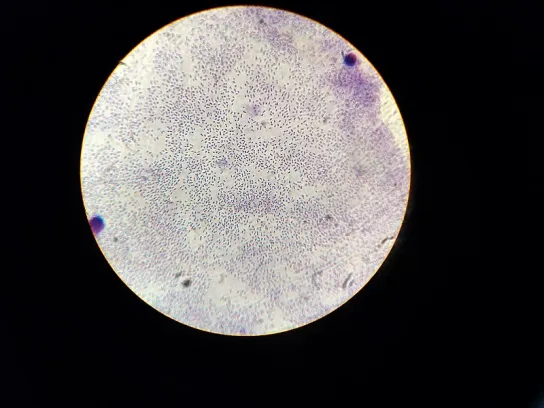
D. pneumoniae is a common pathogen that infects humans’ respiratory tract and can spread via droplets of airborne dust. Their capsule is comprised of polysaccharides which define different serologic forms. They are responsible for virulence as well as pathogenicity. The severity of virulence varies among serologic forms because of genetic variation.
The people who are most susceptible to ailments and infections resulting from D. pneumoniae include those suffering from chronic conditions like cardiorespiratory diseases, diabetes, and liver disease, people who suffer from immunosuppression or immunodeficiency or sickle cell disorders, and anatomical or functional asplenia and people who drink as well as smoking cigarettes.
Difference Between Streptococcus Pneumoniae and Diplococcus Pneumoniae
Taxonomy and Classification
Taxonomy and classification are central principles in biology that facilitate the systematic organization of living organisms based on evolutionary relationships and shared characteristics. Taxonomy involves the study of naming, classifying, and categorizing organisms while classification involves grouping them hierarchically into distinct classes.
Taxonomic ranks, from broad to specific, are Domain, Kingdom, Phylum, Class Order Family Genus, and Species. Each rank denotes different degrees of relatedness between organisms with species being the highest-level unit recognized universally.
Modern taxonomy has advanced beyond morphological observations to use molecular techniques such as DNA sequencing for more accurate classifications and identification of related organisms. This newer approach helps reveal evolutionary history as well as genetic ties among organisms.
Taxonomy provides scientists with a language for communicating clearly and effectively and helps us better comprehend Earth’s vast diversity of life. Taxonomy aids species identification, conservation efforts, and ecological relationships while classification continues to progress and enrich our knowledge of nature.
Morphological Differences
Streptococcus pneumoniae:
- Cell Structure: When observed under a microscope, Streptococcus pneumoniae typically appears as oval-shaped cocci (spherical cells) arranged in chains. Individual cocci can often be found singly or pairwise when observed closely.
- Gram Stain: Streptococcus pneumoniae is a Gram-positive bacteria, meaning it retains violet dye during Gram staining procedures to create its characteristic purple hue when observed under a microscope.
- Capsule: These bacteria commonly possess a protective capsule made up of complex sugars that act as an important virulence factor and contribute to their pathogenicity.
Diplococcus Pneumoniae:
- Cell Structure: Diplococcus Pneumoniae is another cocci bacterium, but can often be seen appearing as pairs – giving them their distinctive diplococcal arrangement in clinical samples.
- Gram Stain: Diplococcus Pneumoniae is a Gram-negative bacteria, meaning that instead of taking up violet stain it takes on red counterstain in the Gram staining process and appears pink or red under a microscope.
- Pili (Fimbriae): This bacteria is well-known for its pili or fimbriae, hair-like appendages on its surface that aid in adhesion to host cells and contribute to pathogenicity. These pili are essential in providing adhesion for pathogenicity as they ensure adhesion.
Clinical Significance
Streptococcus pneumoniae:
- Pneumonia: Pneumococcal pneumonia is one of the primary causes of community-acquired pneumonia (CAP), impacting people of all ages worldwide. Pneumococcal infection may range from mild to severe severity and thus represents a major public health concern worldwide.
- Meningitis: Meningitis-causing bacteria have been responsible for an array of cases in children and seniors alike, often manifesting as meningitis, an inflammation of membranes surrounding the brain and spinal cord.
- Sinusitis and Otitis Media: Streptococcus pneumoniae is one of the primary causes of sinusitis (inflammation of the sinuses) and middle ear infection, particularly among children.
- Invasive Diseases: Additionally, exposure can result in life-threatening invasive diseases like bacteremia (the presence of bacteria in the bloodstream) and septicemia (systemic infection due to bacteria), as well as potential lifelong problems like sepsis.
Neisseria gonorrhoeae:
- Gonorrhea: Neisseria gonorrhoeae is the bacteria responsible for gonorrhea, a sexually transmitted infection (STI). Gonorrhea usually affects both male’s and females genitourinary tracts, leading to symptoms like painful urination, discharge from both female genital organs, as well as more serious health consequences if left untreated.
- Complications: Left untreated, gonorrhea can lead to serious health consequences in both men and women, including pelvic inflammatory disease (PID) in female victims as well as epididymitis in male victims – increasing the risk of HIV transmission.
- Antibiotic Resistance: Neisseria gonorrhoeae has developed resistance to multiple antibiotics, making treatment of gonorrhea more difficult and emphasizing the need for surveillance and antibiotic stewardship programs.
Pathogenesis and Virulence Factors
Streptococcus pneumoniae:
- Capsule: One of the key virulence factors of S. pneumoniae is its polysaccharide capsule. This defense mechanism allows S. pneumoniae to avoid detection by its host’s immune system by avoiding phagocytosis, the process by which immune cells capture and destroy pathogens, while also playing an integral role in its ability to colonize respiratory epithelial cells and adhere to them.
- Pneumolysin: Streptococcus pneumoniae produces pneumolysin, a toxin produced by Streptococcus pneumoniae that can damage host cells such as respiratory epithelial cells and immune cells, contributing to inflammation and tissue damage in the lungs during pneumonia.
- Autolysin: Autolysins are enzymes produced by bacteria to break down their own cell wall, which then releases various bacterial components such as cell wall fragments and DNA into the environment, potentially prompting an inflammatory response and further contributing to disease pathology.
- Neisseria gonorrhoeae: It contains hairlike appendages called Pili, which play an essential role in adhesion to host cells and allow it to infiltrate mucosal surfaces of genital and rectal areas, aiding infection.
- Opa Proteins: Neisseria gonorrhoeae produces Opa (opacity-associated) proteins to assist it in attaching to host cells and modulating immune responses, as well as interacting with host cell receptors for entry and survival within these host cells.
- Antigenic Variation: N. gonorrhoeae exhibits antigenic variation by altering its surface structures to escape detection by immune systems in host nations, making a long-term immune response difficult for hosts. This ability to change surface antigens renders developing long-term immunity difficult.
- Endotoxins: N. gonorrhoeae is one of many Gram-negative bacteria which produce lipopolysaccharides (endotoxins). These endotoxins may trigger an intense inflammatory response in their hosts and contribute to infection symptoms.
Epidemiology and Transmission
Streptococcus pneumoniae:
- Epidemiology: Streptococcus pneumoniae is a widespread bacteria found in healthy upper respiratory tracts of individuals worldwide. It’s one of the major causes of respiratory infections such as pneumonia, accounting for a significant global burden of disease.
- Epidemiological pattern: Epidemiological patterns vary depending on age group, with young children and the elderly more at risk for serious infections than other age groups. This infection causes both community-acquired infections as well as healthcare-associated ones.
Transmission: Person-to-person transmission is the primary mode of spread, usually by respiratory droplets expelled when infected people cough or sneeze, increasing risk. Furthermore, living close to someone who is infected increases this risk exponentially.
Neisseria gonorrhoeae:
- Epidemiology: N. gonorrhoeae is a sexually transmitted bacteria responsible for gonorrhea, an often life-threatening sexually transmitted infection (STI).
- Epidemiology of Gonorrhea: Sexual Behaviour and Practices Its incidence increases among sexually active populations. Geographic and population variations play a part, with higher rates among certain demographics.
- TRANSMITTAL: Neisseria gonorrhoeae can be spread via sexual contact between infected individuals, such as vaginal, anal, or oral sex; or birth-transmitted mother to infant. Neonatal gonorrhea may result from these two transmission routes.
Diagnosis and Laboratory Identification
Streptococcus pneumoniae:
- Gram staining: Gram-positive cocci appear in pairs or chains when stained; this method allows healthcare providers to quickly detect S. pneumoniae infections.
- Culture: Clinical specimens such as sputum, blood, or cerebrospinal fluid can be cultured on agar plates for S. pneumoniae to be grown into colonies on blood agar plates. Alpha-hemolytic colonies will typically form from S. pneumoniae when grown this way.
- Optochin Susceptibility Test: The optochin susceptibility test can help differentiate S. pneumoniae from other streptococci species by testing for its susceptibility to optochin; S. pneumoniae is sensitive while other streptococci aren’t.
- Bile Solubility Test: S. pneumoniae is known to be bile-soluble, meaning it can be digested by bile. To verify this characteristic, perform a bile solubility test.
- Antigen Detection: Immunological tests such as the Quellung Reaction can identify specific capsular antigens of S. pneumoniae for serotyping purposes.
- Molecular Methods: Polymerase Chain Reaction (PCR) techniques can detect specific S. pneumoniae genes or genetic markers for accurate and rapid identification.
Neisseria gonorrhoeae:
- Culture: Culture of N. gonorrhoeae colonies on appropriate media such as Thayer-Martin or modified New City (NYC) agar can isolate them and serve as an essential step for antibiotic susceptibility testing.
- Nucleic Acid Amplification Tests (NAATs): NAATs are highly sensitive and specific molecular tests designed to detect N. gonorrhoeae DNA or RNA in clinical specimens; they are often used for diagnosis when culture may not be feasible.
- Antigen Detection: Enzyme immunoassays (EIAs) or other immunoassays can detect gonococcal antigens present in clinical samples using EIAs or other types of immunoassays.
- Antibiotic Susceptibility Testing: Culture-based methods are indispensable when it comes to testing for antibiotic susceptibility among N. gonorrhoeae strains, given the increasing threat of antibiotic resistance.
- DNA Sequencing: DNA sequencing can often be used to identify specific genetic markers associated with certain strains of N. gonorrhoeae, such as antibiotic resistance.
What is the best treatment for Streptococcus Pneumoniae and Diplococcus Pneumoniae?
Streptococcus pneumoniae:
Treatment:
- Antibiotics: The most commonly used antibiotics to combat illnesses due to S. pneumoniae are penicillin, amoxicillin or macrolides, and ceftriaxone (e.g. azithromycin). The selection of an antibiotic is based on factors like the intensity of illness and the local patterns of resistance to antibiotics.
- The Vaccination Method: Pneumococcal conjugate vaccines (PCVs) similar to Prevnar 13 are utilized to protect against pneumococcal infections both in both adults and children. Vaccination reduces the risk of illness as well as the use of antibiotics.
Antimicrobial Resistance:
- Resistance to antimicrobials within S. pneumoniae has become becoming a major issue. Some strains are resistant to multiple antibiotics, such as macrolides and penicillin.
- Monitoring resistance to antibiotics is crucial to determine the best treatment for antibiotics.
- In certain instances, higher doses or other kinds of antibiotics might be required to fight resistant strains.
Neisseria gonorrhoeae:
Treatment:
- Antibiotic treatment: currently recommended for gonorrhea that is not complicated is dual therapy that includes ceftriaxone (an injectable cephalosporin) as well as azithromycin (an oral macrolide). This combination is intended to ensure an effective treatment and decrease the chance of developing resistance.
- Tests for Antibiotic Susceptibility: Due to rising concerns over resistance, it’s essential to conduct tests for susceptibility to antibiotics to help guide the decision-making process.
Antimicrobial Resistance:
- Neisseria Gonorrhoeae is resistant to several types of antibiotics, such as penicillins, tetracyclines, as well as fluoroquinolones.
- The emergence of ceftriaxone-resistant strains is a major concern, making it the last effective option for treating gonorrhea.
- Continuous monitoring of resistance to antimicrobials and research into the development of new treatments are essential to combating this health risk to the public.
Prevention and Vaccination of Streptococcus Pneumoniae and Diplococcus Pneumoniae
Streptococcus pneumoniae (Pneumococcus):
- Pneumococcal Conjugate Vaccines (PCVs): PCVs such as Prevnar 13 (PCV13) and Synflorix offer protection from various strains of S. pneumoniae responsible for various illnesses like pneumonia, meningitis, and otitis media. Infants, young children and older adults should receive PCVs regularly.
- Pneumococcal Polysaccharide Vaccine (PPSV): Pneumovax 23 is an adult vaccine recommended for those aged 65 and over as well as individuals with certain medical conditions, providing protection from an array of S. pneumoniae serotypes.
- High-Risk Group Vaccinations: People in specific medical conditions, such as immunocompromised individuals or those living with chronic illnesses, may receive pneumococcal vaccines as part of their healthcare plan.
Neisseria meningitidis (Diplococcus pneumoniae): This organism causes meningitis.
Neisseria meningitidis is widely recognized for causing meningococcal infections such as meningitis and septicemia, making vaccination an integral part of protecting against such threats. Vaccination should always be considered when trying to avoid such illnesses:
- Meningococcal Conjugate Vaccines (MCVs): MCVs such as MenACWY (Menactra or Menveo) provide protection from serogroups A, C, W, and Y of N. meningitidis; these vaccinations should be considered among adolescents, college students and individuals at higher risk for meningococcal disease.
- Meningococcal B Vaccines: Meningococcal B vaccines such as Bexsero and Trumenba provide protection from serogroup B of N. meningitidis; they are highly recommended for individuals at increased risk or in outbreak situations.
- Travel Vaccination: Travelers traveling to regions with high rates of meningococcal disease may require specific vaccines tailored to the predominant serogroups found there.
- Vaccination during Outbreaks: When outbreaks of meningococcal disease arise, vaccination campaigns may be conducted against affected populations to curb its spread and control its impact.
Summary
Pneumonia is an acute respiratory infection affecting the lungs. Two bacteria responsible are Streptococcus pneumoniae and Diplococcus pneumoniae; Streptococcus exists as chains of cocci cells while Diplococcus exists as pairs.
This distinction makes Streptococcus pneumoniae distinct from Diplococcus. Both organisms possess Gram-positive properties with round shapes commonly found within the respiratory tract.

