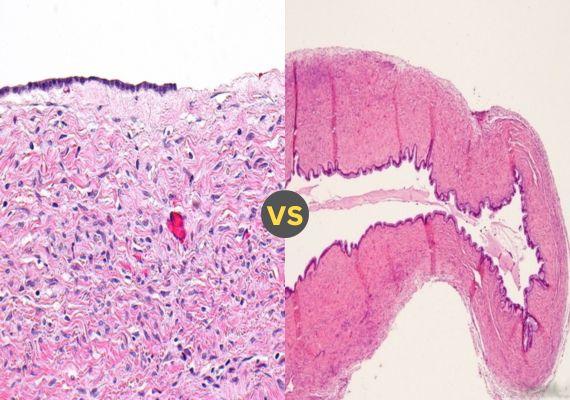
Introduction of Serous and Mucinous Cystadenoma of Ovary
Serous and Mucinous Cystadenoma of Ovary are noncancerous ovarian cysts that frequently affect women. Both types originate in the surface epithelium of the ovary and typically present themselves as fluid-filled sacs although both share some similarities, there are key distinctions between them.
Serous cystadenomas are characterized by cysts filled with thin, watery fluid that gives the cyst its multilocular appearance and are typically smaller in size and asymptomatic, when symptoms do present themselves they may include abdominal discomfort or pain.
Mucinous cystadenomas contain thicker mucus-like fluid, giving them a larger and rounder shape than their serous counterparts. While serous cystadenomas tend to remain small over time, mucinous ones can grow quite large over time and lead to abdominal distension and discomfort as well as more serious complications like ovarian torsion or rupture.
Distinguishing between serous and mucinous cystadenomas is key for effective diagnosis and treatment planning. Treatment options range from watchful waiting to surgical removal depending on size, symptoms and potential complications associated with each type of benign ovarian cyst. Regular medical follow-up should also be undertaken for best health results.
What is Serous Cystadenoma of Ovary?
Serous cystadenoma of the ovary is a fluid-filled benign tumor originating from its surface epithelium. This type of cyst can be distinguished by an excess proliferation of serous epithelial cells similar to those found in fallopian tubes. Typically forming sac-like structures filled with clear, watery fluid. They may present as single or multilocular (multiple compartments).
-
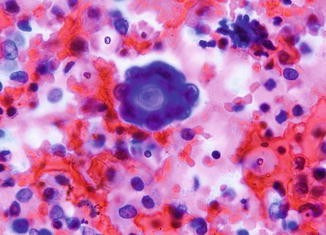
Figure 01: Serous Cystadenoma of Ovary
Serous cystadenomas of the ovary are among the most frequently occurring types of benign ovarian tumors, often occurring unknowingly during routine pelvic exams or imaging studies. When they do cause symptoms, this usually stems from their size causing abdominal discomfort or pain.
Serous cystadenomas of the ovary are typically noncancerous (benign), with favorable prognoses and recommended management by conservative approaches such as regular monitoring. If cysts become large or cause symptoms or malignancy is suspected, surgical removal may be advised in certain instances. Accurate diagnosis and appropriate management are paramount in ensuring the well-being of individuals living with serous cystadenomas of their ovary.
Characteristics of Serous Cystadenoma of Ovary
Serous cystadenoma of the ovary is a benign ovarian tumor with specific characteristics.
Here are the key traits associated with serous cystadenomas:
- Epithelial Origin: Serous cystadenomas have their source in the ovarian surface epithelium and in particular from serous epithelial cells that line its surface, producing clear, thin watery fluid that eventually accumulates as cystadenomas.
- Fluid Content: Cysts that contain serous or transparent fluid give these cysts their distinctive, watery look.
- Cyst Structure: Serous cystadenomas usually take the form of smooth-walled cysts with thin walls that may also be multilocular – meaning multiple compartments or chambers exist within a cyst.
- Size: Serous cystadenomas come in all shapes and sizes, but are typically smaller compared to their mucinous counterparts. Their sizes can range from several centimeters up to larger sizes.
- Symptoms: Many serous cystadenomas are asymptomatic, meaning that they do not produce noticeable symptoms. When symptoms do present themselves, however, they tend to correlate with the size and type of cyst present and may include mild abdominal discomfort or pain.
- Complications: Serous cystadenomas tend to cause less serious side effects, including ovarian torsion (twisting of the ovary) or rupture, than other types of ovarian cysts.
- Treatment Options for Serous Cystadenomas: Options for treating serous cystadenomas depend on factors like their size, symptoms and overall health of the patient. Small, asymptomatic cysts may be monitored conservatively with regular monitoring while larger or symptomatic cysts may require surgical removal.
- Prognosis: Serous cystadenomas tend to be benign and carry an excellent prognosis; with proper treatment or surveillance, most individuals can expect an excellent outcome.
What is Mucinous Cystadenoma of Ovary?
Mucinous cystadenoma of the ovary is a benign tumor originating from surface epithelial cells of the ovary and characterized by the proliferation of mucinous epithelial cells that produce thick gel-like or mucus-like fluid. These cells then form cystic structures within the ovary which often result in cysts of various sizes; some cysts even become quite large over time.
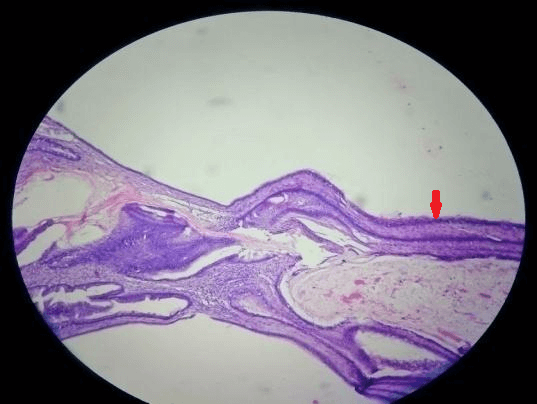
Mucinous cystadenomas can be identified by their viscous fluid, which resembles mucus. They often present as multilocular (with multiple compartments) growths with septations or internal partitions separating compartments.
Mucinous cystadenomas can present symptoms when they reach significant sizes, including abdominal distension, discomfort, and pain. Furthermore, these cysts may exert pressure on surrounding organs which could potentially lead to complications like ovarian torsion (twisting of the ovary) or cyst rupture.
Although mucinous cystadenomas are generally benign, they do carry an increased risk of malignancy than serous cystadenomas and must therefore be diagnosed and managed accurately to reduce this risk. Treatment options may include surgical removal for larger cysts that become symptomatic or when there is evidence of malignancy; medical follow-up is also crucial to ensure the well-being of affected individuals.
Characteristics of Mucinous Cystadenoma of Ovary
Mucinous cystadenoma of the ovary is an unusual, benign ovarian tumor with several distinctive characteristics:
- Epithelial Origin: Mucinous cystadenomas form in ovarian surface epithelium cells known as the mucinous epithelial cells, which produce thick, gel-like or mucus-like fluid.
- Fluid Content: Cysts composed of viscous or viscerally thick fluid have an interesting appearance and texture due to their fluid-filled interior, giving these cysts their distinctive look and texture.
- Structure: Mucinous cystadenomas typically present as thick-walled cysts compared to serous cystadenomas, often with rounded shapes and the presence of septations or internal partitions that create multilocular effects.
- Size: Mucinous cystadenomas may reach significant sizes; typically larger than serous cystadenomas. Their sizes can range from several centimeters up to considerable sizes.
- Symptoms: Mucinous cystadenomas tend to produce symptoms when they grow large, including abdominal distension, discomfort and pain. Furthermore, pressure from these cysts may exert itself onto nearby organs leading to gastrointestinal or urinary symptoms.
- Complications: Mucinous cystadenomas carry the risk of serious complications, including ovarian torsion due to their size or cyst rupture that leads to peritonitis (inflammation of the abdominal lining).
- Treatment Options for Mucinous Cystadenomas: Options vary based on factors like their size, symptoms, and overall health status of a patient. Surgery may be recommended in cases involving larger cysts that are symptomatic, or when malignancy is suspected.
- Prognosis: Mucinous cystadenomas tend to be harmless but have an increased risk of malignancy compared with serous cystadenomas, so proper diagnosis and management are critical in order to provide effective treatment and rule out any potential malignant potential.
Key Difference Between Serous and Mucinous Cystadenoma of Ovary
Here’s a comparison chart highlighting the key differences between Serous Cystadenoma and Mucinous Cystadenoma of the Ovary:
| Characteristic | Serous Cystadenoma | Mucinous Cystadenoma |
|---|---|---|
| Type of epithelial cells | Serous epithelial cells | Mucinous epithelial cells |
| Fluid content | Thin, watery fluid | Thick, gel-like or mucus-like fluid |
| Appearance of cysts | Smooth, often multilocular | Larger, rounded, may have septations |
| Size | Typically smaller | Can be larger |
| Symptoms | Often asymptomatic; when symptomatic, may cause abdominal discomfort or pain | More likely to cause symptoms, including abdominal distension and discomfort |
| Complications | Less likely to cause complications | May lead to complications like ovarian torsion or cyst rupture |
| Surgical removal | Required for larger or symptomatic cysts | Typically required for larger cysts, symptomatic cases, or when malignancy is suspected |
| Prognosis | Usually benign and associated with a good prognosis | Typically benign, but there’s a higher risk of malignancy compared to serous cystadenomas |
Diagnostic and Treatment
Diagnostic Tests of Serous and mucinous cystadenomas
Serous and mucinous cystadenomas of the ovary can be diagnosed through clinical evaluation, imaging studies, laboratory tests and surgical intervention.
Here are the primary diagnostic tools and methods used to detect such cysts:
Clinical Evaluation:
- Medical History: This will allow us to understand a patient’s symptoms, risk factors, and related medical conditions more fully.
- Physical Examination: A pelvic exam may reveal abdominal masses or tenderness.
Imaging Studies:
- Ultrasound: Transvaginal or abdominal ultrasound imaging is one of the best tools available to detect ovarian cysts, providing details such as their size, location and characteristics.
- CT Scan or MRI: These imaging techniques may be beneficial when ultrasound results are inconclusive or when more information is necessary in evaluating the characteristics of cysts.
Laboratory Tests:
- CA-125 Blood Test: This tumor marker may be elevated in some ovarian tumors, including malignant ones, but its level doesn’t solely correlate to cancer; instead it could also indicate endometriosis.
- Cyst Fluid Analysis: Once aspirated from or removed surgically, cyst fluid can be tested for specific characteristics that help differentiate benign from malignant cysts.
Biopsy and Surgical Interventions:
- Surgery (Biopsy): For definitive diagnosis of serous and mucinous cystadenomas, surgery may be necessary (cystectomy or oophorectomy). Tissue samples obtained during these procedures will then be examined under a microscope by a pathologist in order to confirm its type and benign nature.
While imaging and blood tests can provide valuable information, definitive diagnosis of serous or mucinous cystadenomas usually relies on histological examination of tissue samples obtained through surgery. Furthermore, accurate diagnosis by healthcare providers is key in order to provide patients with appropriate treatments and patient care.
Treatment options for serous and mucinous cystadenomas
- Serous Cystadenomas: Watchful Waiting: For small and asymptomatic serous cystadenomas that do not present symptoms, conservative management may include monitoring by imaging studies (ultrasound or MRI) and blood tests (CA-125). If they remain stable without symptoms developing, immediate intervention may not be required.
- Surgical Removal (Cystectomy): For larger serous cystadenomas that cause symptoms or have suspicious features, surgery may be the answer. Laparoscopic or laparotomy techniques may be employed; either way, cystectomy involves extracting the cyst while leaving healthy ovarian tissue undamaged by its removal.
- Follow-Up Appointments: Once surgical removal, regular follow-up appointments should be scheduled in order to monitor the patient’s condition and ensure no recurrence or complications arise.
- Mucinous Cystadenomas: Surgical Removal (Cystectomy or Oophorectomy): When left untreated, Mucinous cystadenomas have the potential to grow to significant sizes and cause symptoms, often necessitating surgery for removal. For larger cysts that cause symptoms or when malignancy is suspected or confirmed; surgery (usually cystectomy or oophorectomy) may also be recommended in these instances.
- Pathological Examination: Tissue samples taken from removed cysts will be sent for pathological analysis in order to confirm diagnosis, rule out malignancy and identify their nature and type.
- Follow-Up Appointments: It is imperative after surgery for patients to attend regular follow-up appointments in order to assess their condition and detect any recurrences or complications that might arise from treatment.
Summary
Serous cystadenomas and mucinous cystadenomas of the ovary are two distinct benign tumors, each producing their own thin watery liquid that typically presents itself in small, smooth cysts that often remain asymptomatic. Mucinous cystadenomas differ by producing thicker, mucus-like fluid, leading to larger, rounder cysts which may cause abdominal discomfort and distension.
Mucinous cystadenomas carry a higher risk of complications, including ovarian torsion or cyst rupture, as well as an elevated risk of malignancy than serous cystadenomas. For both types, surgical removal may be necessary depending on size, symptoms, and suspicion of malignancy with generally positive prognoses when managed appropriately.