Introduction of Pityriasis Versicolor and Vitiligo
Pityriasis Versicolor and Vitiligo lie in the alteration of skin pigmentation, causing patches that differ in color from the surrounding skin.
Skin conditions can be bewildering, especially when their appearances are deceptively similar. Pityriasis versicolor and vitiligo are two such skin disorders that can perplex both patients and onlookers due to their superficial resemblance.
Pityriasis versicolor is a fungal infection characterized by scaly, discolored patches, while vitiligo is an autoimmune disorder marked by the development of well-defined, white patches on the skin.
We will delve into the distinct characteristics of these conditions, elucidating their definitions, causes, and symptoms, facilitating a better understanding of the disparities between them.
What is Pityriasis Versicolor?
Pityriasis versicolor, also known as tinea versicolor, is a common fungal skin infection caused by the yeast Malassezia. This yeast is a natural inhabitant of the skin’s microbiome, but under certain circumstances, it can proliferate excessively, leading to the development of pityriasis versicolor.
The condition is typically characterized by the presence of scaly, discolored patches on the skin’s surface, often appearing on the chest, back, and upper arms.
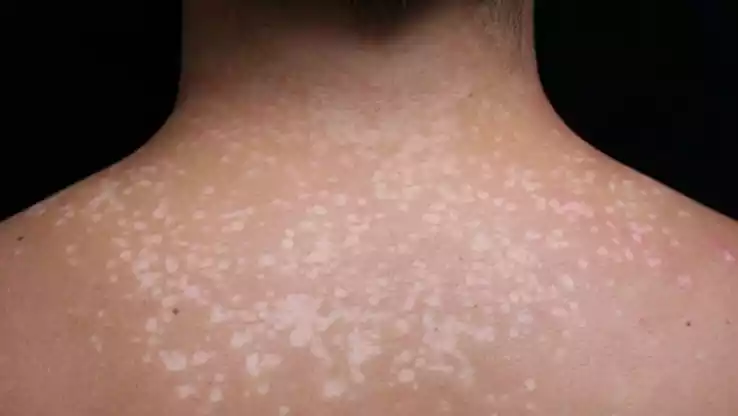
Pityriasis versicolor manifests in various colors, including pink, white, tan, or brown, depending on the individual’s skin type and the stage of the condition. Some individuals with this fungal infection may experience mild itching and, in rare cases, minor skin irritation.
The distinctive appearance of these scaly patches is due to the disruption of normal melanin production on the affected skin, resulting in pigmentary variations.
Types of Pityriasis Versicolor
- Hypopigmented Type: This is the most common form, characterized by the development of light-colored patches on the skin. These patches are usually lighter than the surrounding skin and can range in color from white to pink or light brown.
- Hyperpigmented Type: In this variant, the affected areas of the skin develop darker pigmentation compared to the surrounding skin. These patches can appear light brown to dark brown and may cause cosmetic concerns, especially in individuals with lighter skin tones.
What is Vitiligo?
Vitiligo is a chronic autoimmune skin disorder characterized by the gradual loss of skin pigmentation, resulting in the formation of well-defined, depigmented, white patches.
This condition arises when the immune system erroneously attacks and destroys melanocytes, the pigment-producing cells present in the epidermis. The resulting depigmentation is often most noticeable in individuals with darker skin tones.

Vitiligo’s etiology remains complex and not entirely understood, but it is thought to have a genetic component. Environmental factors, such as trauma, sunburn, and stress, can trigger or exacerbate vitiligo in susceptible individuals.
Contrary to other skin conditions, vitiligo patches are devoid of melanin, making them starkly white against the patient’s natural skin tone.
Types of Vitiligo
- Non-segmental Vitiligo: This form is the most common type of vitiligo and is characterized by the symmetric loss of pigmentation on both sides of the body. It often affects areas such as the hands, face, and body folds, and can progress slowly or rapidly over time.
- Segmental Vitiligo: This type is less common and usually occurs at a younger age. It is characterized by the loss of pigmentation in a specific segment or area of the body. Segmental vitiligo may progress for a limited time and then remain stable, affecting only one side of the body.
Causes and Symptoms
Pityriasis versicolor is primarily caused by the overgrowth of the yeast Malassezia, which is normally present on the skin. It thrives in warm, humid conditions, making individuals in such environments more susceptible.
Excess sebum production, often seen in individuals with oily skin, can also contribute to the proliferation of this yeast. Weakened immune systems, as observed in individuals with conditions like HIV or those taking immunosuppressive medications, can predispose individuals to pityriasis versicolor.
Symptoms typically include the development of scaly, discolored patches on the chest, back, and upper arms, often accompanied by mild itching and occasional skin irritation.
Vitiligo, on the other hand, is an autoimmune disorder where the immune system mistakenly targets and destroys melanocytes. Genetic predisposition plays a significant role in its development, and environmental factors such as trauma, sunburn, and stress may trigger or exacerbate the condition.
The hallmark symptoms are well-defined, white patches on various areas of the body, including the face, hands, and extremities. Hair in the affected areas may also lose pigmentation and turn white, and there is typically no associated itching or discomfort.
How Pityriasis Versicolor and Vitiligo Start and Progress
Pityriasis Versicolor: Pityriasis versicolor typically begins with the overgrowth of the yeast Malassezia, which is naturally present on the skin. Factors such as warm and humid climates, excessive sweating, or oily skin can create an environment conducive to yeast proliferation.
The overgrown yeast disrupts the normal pigmentation process, leading to the development of scaly, discolored patches on the skin. If left untreated, these patches can gradually spread and merge, resulting in larger affected areas.
In some cases, the condition can recur, especially in individuals with predisposing factors such as weakened immune systems or those living in tropical regions.
Vitiligo: The onset of vitiligo is attributed to an autoimmune process where the body’s immune system mistakenly attacks and destroys melanocytes, the pigment-producing cells in the skin.
The exact triggers for this autoimmune response are not fully understood, although genetic predisposition and environmental factors such as stress, sunburn, or chemical exposure may play a role.
Vitiligo can start with small, localized depigmented patches that may gradually expand over time, affecting larger areas of the skin. The progression of vitiligo can be unpredictable, with periods of stability followed by episodes of rapid depigmentation.
Difference Between Pityriasis Versicolor and Vitiligo
Here’s a comparison chart for Pityriasis Versicolor and Vitiligo:
| Aspect | Pityriasis Versicolor | Vitiligo |
|---|---|---|
| Microbiological Aspect | Fungal overgrowth (Malassezia) | Autoimmune attack on melanocytes |
| Appearance | Scaly patches, variable colors, can itch | Well-defined white patches, non-itchy |
| Affected Areas | Often chest, back, upper arms | Various, including face, hands, body folds |
| Onset and Progression | Gradual onset, patches may spread | Variable onset, patches expand over time |
| Diagnosis Methods | Clinical examination, microscopy | Clinical examination, occasional skin biopsy |
| Primary Treatment | Antifungal creams or oral medications | Corticosteroids, phototherapy, immunosuppressants |
| Preventive Measures | Maintain good hygiene, control sweating | Minimize skin trauma, sun protection |
| Epidemiological Prevalence | Common fungal infection, more prevalent in humid regions | Less common autoimmune condition, affects all climates |
| Psychological Impact | Typically less emotionally distressing | Often associated with emotional challenges |
| Typical Age of Onset | Adolescence and early adulthood | Can manifest at any age, including childhood |
| Types (if applicable) | Hypopigmented and hyperpigmented | Non-segmental and segmental forms |
What is the similarity between Pityriasis Versicolor and Vitiligo?
Pityriasis versicolor and vitiligo are two skin conditions that, at first glance, may appear similar due to changes in skin pigmentation, but they have some key differences. Here are a few similarities between Pityriasis Versicolor and Vitiligo:
- Skin Pigmentation Changes: Both conditions manifest as changes in skin pigmentation, resulting in patches that are lighter or darker than the surrounding skin.
- Cosmetic Concerns: Both conditions can be cosmetically bothersome, causing individuals to be self-conscious about the appearance of their skin.
- Psychological Impact: The altered skin pigmentation in both Pityriasis versicolor and vitiligo can lead to psychological distress, affecting self-esteem and confidence.
- Dermatological Evaluation: To diagnose both conditions accurately, a dermatologist’s evaluation is usually necessary, as the clinical presentation can be similar.
- Patchy Skin: Both conditions present as patches on the skin, which can vary in size and distribution.
- Chronic Nature: Pityriasis versicolor and vitiligo are chronic conditions, meaning they can persist over time and may require ongoing management.
- Patient Awareness: Affected individuals may become more aware of their skin’s appearance and seek treatment for cosmetic reasons, not just medical ones.
- Overlap in Affected Areas: Although the typical locations for these conditions differ, both Pityriasis versicolor and vitiligo can occur on various parts of the body.
- Potential for Misdiagnosis: The similarities in skin pigmentation changes can sometimes lead to misdiagnosis, underscoring the importance of consulting a dermatologist.
- Support Networks: People with both conditions may find support and advice from patient advocacy groups and support networks that cater to individuals with skin conditions and body image concerns.
Diagnosis and Treatment
Pityriasis Versicolor: Diagnosing pityriasis versicolor typically involves a visual examination of the affected areas by a healthcare provider. To confirm the diagnosis, skin scrapings may be collected and examined under a microscope to identify the presence of Malassezia yeast.
Once diagnosed, treatment options vary based on severity. Mild cases can often be managed with over-the-counter antifungal creams, while more severe or recurrent cases may require prescription-strength topical or oral antifungal medications.
It is also essential to address factors promoting yeast growth, such as wearing loose clothing, avoiding excess sweating, and using antifungal shampoos in affected areas.
Vitiligo: Diagnosing vitiligo is generally straightforward, relying on a physical examination and, in some cases, a skin biopsy. Treatment for vitiligo aims to repigment the affected areas or slow down the spread of depigmentation.
Therapies include topical corticosteroids, phototherapy (light therapy), and immunosuppressive agents. For those who don’t respond to these treatments, surgical options like skin grafting or tattooing may help to mask the depigmented areas.
Prevention
Pityriasis Versicolor: Preventing pityriasis versicolor involves primarily reducing factors that promote yeast overgrowth:
- Maintain Good Hygiene: Regularly cleanse and dry your skin, particularly in areas prone to sweat and oil buildup, such as the chest and back.
- Wear Loose-Fitting Clothing: Loose and breathable clothing helps reduce humidity and sweating, creating an unfavorable environment for yeast growth.
- Use Antifungal Shampoos: In areas prone to infection, like the scalp, using antifungal shampoos can help control yeast growth and prevent recurrences.
- Avoid Excessive Sweating: If you engage in activities that cause excessive sweating, shower promptly afterward and consider using talcum powder to keep the skin dry.
- Minimize Oily Skin: If you have naturally oily skin, consider using non-comedogenic skincare products to help reduce excess sebum production.
- Avoid Sharing Personal Items: To prevent the spread of the yeast to others, avoid sharing personal items like towels and clothing.
Vitiligo: Preventing the onset of vitiligo is challenging since it is primarily an autoimmune disorder. However, there are steps to minimize environmental triggers and manage the condition:
- Minimize Skin Trauma: Protect your skin from cuts, burns, and other forms of trauma to reduce the risk of new depigmented areas developing.
- Sun Protection: UV exposure can worsen vitiligo, so wearing sunscreen and protective clothing is crucial to prevent further depigmentation.
- Stress Management: Chronic stress may exacerbate autoimmune conditions. Engage in stress-reduction techniques such as meditation, yoga, or counseling.
- Regular Medical Checkups: Routine medical checkups can help identify vitiligo early and monitor its progression. Early intervention may slow down depigmentation.
- Camouflage Techniques: Cosmetics and camouflage products can help conceal depigmented areas, improving self-esteem and reducing emotional stress associated with vitiligo.
Summary
Pityriasis versicolor and vitiligo, though visually similar in some aspects, differ significantly in their causes, symptoms, diagnosis, and treatment. Pityriasis versicolor results from yeast overgrowth, causing scaly, discolored patches often on the chest and back, with mild itching.
Treatment includes antifungal measures. In contrast, vitiligo is an autoimmune disorder that leads to well-defined white patches devoid of pigmentation. There is no associated itching, and treatment focuses on repigmentation or halting depigmentation spread.
Prevention strategies also differ, with antifungal measures for pityriasis versicolor and minimal environmental triggers for vitiligo. Understanding these distinctions is critical for accurate diagnosis and tailored treatment.

