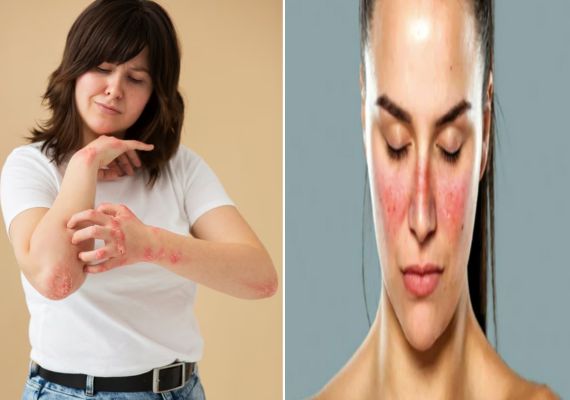
Overview of Lichen Planus and Lupus Erythematosus
Lichen Planus and Lupus Erythematosus are autoimmune conditions that can manifest with skin and mucous membrane involvement.
Lichen Planus, also known as Chronic Inflammatory Skin and Mucosal Disorder (CISKMD), is a chronic inflammatory skin and mucosal condition characterized by itchy, flat-topped purplish papules and lesions on both the skin, mouth and other mucous membranes, including inside of the mouth or other mucous membranes. While its exact cause remains unknown, experts believe immune system dysfunction could play a part.
Typically diagnosed through clinical examination and biopsy; treatment options typically include topical corticosteroids, immunosuppressants or antihistamines to alleviate symptoms and ease symptoms if necessary although complications could potentially arise with severe cases.
Lupus Erythematosus (LLE) refers to a group of autoimmune diseases, with Systemic Lupus Erythematosus being the most prevalent form. Lupus can affect various body systems including skin, joints and internal organs and is typically marked by skin rashes, joint pain, fatigue, and systemic inflammation.
Diagnosis typically uses clinical criteria and laboratory tests while treatment includes anti-inflammatory medication and immunosuppressants; due to its severe impact Lupus can significantly limit life experiences.
While management requires ongoing medical care as well as lifestyle adjustments to manage symptoms effectively while prevent flare-ups; early diagnosis and treatment are essential in managing both conditions effectively.
What is Lichen Planus
Lichen Planus is an extremely common chronic, inflammatory skin condition that also impacts mucous membranes inside of mouth and genital areas. It manifests itself by producing itchy, flat-topped papules or lesions with purplish or reddish-brown colors ranging from purplish-brown to purplish-red.
Lichen Planus remains unclear in its exact cause, though many believe that an autoimmune response plays a part. Certain triggers, such as medications, infections or stress may predispose individuals to this condition and further accelerate its spread.
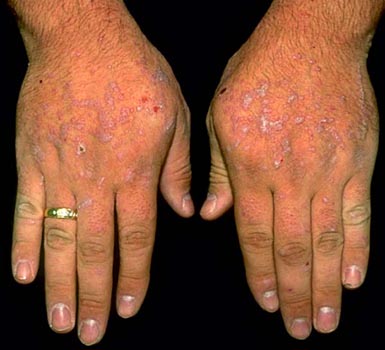
Lichen Planus can usually be diagnosed through clinical examination and, in certain instances, biopsies to confirm its characteristic changes to skin or mucous membrane tissue. Lichen Planus can cause itching that makes living uncomfortable as well as complications when it affects mucosal areas causing discomfort with eating, speaking or sexual activity.
Lichen Planus treatment aims to alleviate symptoms and may include topical corticosteroids, immunosuppressant drugs, antihistamines to ease itching, and oral rinses for mouth lesions.
Though Lichen Planus is generally not a serious condition, managing it effectively requires long-term medical monitoring to maintain control and prevent flare-ups.
What is Lupus Erythematosus
Lupus Erythematosus, or Lupus for short, is an autoimmune condition that impacts many areas of the body. Lupus can manifest in two main forms: Systemic Lupus Erythematosus (SLE) and Cutaneous Lupus Erythematosus (CLE). SLE is a more severe form, involving chronic inflammation that affects skin, joints, kidneys, heart, lungs, brain cells and other organs.
Symptoms may include fatigue, joint pain, skin rashes (often forming a butterfly shape on cheeks and nose), photosensitivity, fever and kidney problems. Diagnosing chronic lymphedema involves specific criteria and laboratory tests.

Treatment typically entails medications to suppress the immune system and reduce inflammation. Furthermore, chronic lymphedema typically impacts skin lesions through various types of rashes and lesions.
Lupus Erythematosus (Lupus) is thought to be caused by genetic and environmental triggers and requires multidisciplinary care from specialists such as rheumatologists and dermatologists for comprehensive management. Early diagnosis and appropriate management are vitally important in order to achieve successful results for individuals living with Lupus.
Symptoms and Causes
Symptoms of Lichen Planus:
- Lichen Planus can be defined by several symptoms that primarily manifest themselves on the skin and mucous membranes:
- Skin Lesions: Lichen Planus often manifests itself in the form of flat-topped, purplish or reddish-brown papules or lesions on the skin that often have polygonal or angular shapes and may form clusters.
- Mucous Membranes Affected: Lichen Planus is known to affect mucous membranes in both the mouth (Oral Lichen Planus) and genital area, often leading to white lacy patches, painful sores or ulcers in those affected.
- Itching: An itchy skin condition can range from mild to severe and often worsens during the night hours.
- Changes to Nails: Nails may sometimes become brittle, ridged or develop grooves over time.
Causes:
Lichen Planus’ exact causes remain poorly understood, although many theories speculate on an autoimmune process being involved, possibly triggered by various external agents like stress or chemicals in the environment:
- Autoimmune Response: Lichen Planus may result from an autoimmune response in which your own immune system mistakenly attacks its own tissues, leading to inflammation and tissue damage.
- Gene Predisposition: There may be a genetic predisposition for Lichen Planus as it tends to run in families.
- Environmental Triggers: Certain medications, infections, allergens or stressors may trigger or exacerbate Lichen Planus symptoms in those predisposed.
- Hepatitis C Infection: Lichen Planus may sometimes be linked with Hepatitis C infection.
Lupus Erythematosus: Its Causes and Symptoms:
Symptoms: Lupus Erythematosus (LE) encompasses an extensive array of symptoms. There are two primary forms.
Systemic Lupus Erythematosus (SLE) and Cutaneous Lupus Erythematosus (CLE):
Systemic Lupus Erythematosus (SLE):
- Skin Rashes: From butterfly rash across cheeks and nose to arthritis-like joint swelling and stiffness.
- Joint Pain: Joint swelling can often mimic arthritis symptoms; additionally fatigue is persistent and extreme while photosensitivity refers to skin sensitivity to sunlight exposure during disease flare-ups.
- Fever: Unexplained fever occurs unexpectedly.
- Kidney Problems: Swelling in the legs, high blood pressure and changes to urine output.
- Neurological Symptoms: Cognitive difficulties, headaches and seizures.
- Hematological Concerns: Anemia, low white blood cell count and platelet count deficiencies.
Cutaneous Lupus Erythematosus (CLE):
Causes:
Lupus Erythematosus remains unknown with its exact causes being unknown but believed to be multifactorial:
- Genetic Predisposition: Genetic factors play an integral part of asthmatic susceptibility; symptoms often run in families.
- Hormonal Influence: Hormone fluctuations, particularly among women, can play an integral role in disease activity. Lupus is more prevalent among those of childbearing age than any other age group.
- Environmental Triggers: Factors like infections, ultraviolet (UV) light exposure and certain medications can all play a part in exacerbating or initiating Lupus symptoms for individuals susceptible to the disease.
- Autoimmune Dysfunction: Lupus is an autoimmune condition wherein the immune system attacks healthy tissues and organs, leading to inflammation and tissue damage. Autoantibodies produced by this immune response contribute significantly to this disease process.
Diagnosis and Tests
Diagnose and Test for Lichen Planus:
- Clinical Exam: To evaluate skin lesions and any mucous membrane involvement, a dermatologist or healthcare provider will conduct an in-depth physical exam.
- Biopsy: For accurate diagnosis of Lichen Planus, a skin biopsy may be required. During this procedure, a small piece of the affected skin or mucous membrane tissue is taken and sent off to a laboratory for microscopic examination. Lichen Planus typically displays characteristic sawtoothed epidermal changes.
Diagnosis and Tests for Lupus Erythematosus (LE), particularly Systemic Lupus Erythematosus (SLE):
Clinical Evaluation: Healthcare providers will perform an in-depth medical history review and physical exam on patients to detect common signs, such as skin rashes, joint pain or any systemic symptoms that could indicate illness or disease.
Laboratory Tests:
- Antinuclear Antibody (ANA) Test: This blood test checks for antibodies that target cell nuclei. While positive ANA tests are common among SLE sufferers, they do not indicate an illness specific result.
- Complete Blood Count (CBC): This test evaluates red and white blood cells as well as platelets to detect anemia or any abnormalities seen with SLE.
- Kidney Function Tests: Lupus can affect kidneys, so blood and urine tests to assess their function such as serum creatinine measurements or urine protein measurements are conducted to accurately gauge their performance.
- Erythrocyte Sedimentation Rate (ESR) and C-reactive Protein (CRP): Elevated levels of these markers may indicate inflammation within the body, as is often found with SLE.
- Complement Levels: Measuring complement proteins C3 and C4 can help track disease activity; low levels may signal disease activity.
Autoantibody Tests:
- Anti-dsDNA Antibodies: Anti-double-stranded DNA antibodies are characteristic of SLE and often associated with more severe disease.
- Anti-Sm Antibodies: Sm antibodies are highly specific for SLE.
- Anti-Ro (SSA) and Anti-La (SSB) Antibodies: These antibodies have been associated with photosensitivity, and may be present in SLE. As additional tests, a dermatological biopsy of affected skin may provide insight into whether or not you have CL.
- Kidney Biopsy: If kidney involvement is suspected, a biopsy can be conducted to assess the extent of damage.
Management and Treatment
Lichen Planus Treatment Options:
- Topical Corticosteroids: Mild to moderate cases of Lichen Planus on skin or mucous membranes are often treated with topical corticosteroid creams or ointments that contain corticosteroids to decrease inflammation, itching and discomfort. These treatments may help decrease inflammation while simultaneously relieving symptoms like itching.
- Oral Corticosteroids: For severe cases or when extensive mucous membrane involvement occurs, oral corticosteroids may be prescribed in order to control symptoms and inflammation.
- Immunosuppressant Medication: When corticosteroids do not prove effective or are poorly tolerated, immunosuppressant drugs like methotrexate, cyclosporine or mycophenolate mofetil may be prescribed to suppress an immune response and limit swelling.
- Topical or Oral Antihistamines: Antihistamines can provide immediate relief of itching and discomfort.
- Oral Rinses and Gels for Lichen Planus: For oral Lichen Planus, rinses or gels containing corticosteroids or other medications may be recommended as solutions.
- Light Therapy (Phototherapy): Light therapy may be effective at treating skin lesions when other methods have proven ineffective. When this approach fails, UV light therapy could potentially provide another means of relief.
- Avoid Triggers: By identifying and avoiding potential triggers such as medication or oral hygiene products that might set off flare-ups, it may help avoid flare-ups altogether.
- Long-Term Monitoring and Adjustments: For long-term management of acne, regular follow up visits with a dermatologist or healthcare provider are often necessary in order to track progress of treatment and adjust it as necessary.
Management and Treatment of Lupus Erythematosus (LE), particularly Systemic Lupus Erythematosus (SLE):
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): For relieving joint pain and inflammation.
- Corticosteroids: Such as prednisone, to manage inflammation and minimize organ damage.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Hydroxychloroquine and Methotrexate can help control symptoms and avoid disease flare-ups, while immunosuppressants like Azathioprine or Mycophenolate Mofetil may be utilized to suppress immune systems in severe cases.
- Biologic Therapies: Biologic drugs may be recommended for more severe or refractory cases of SLE.
- Sun Protection: To safeguard their well-being in light of SLE-related photosensitivity, individuals are recommended to protect themselves with sunscreen use and protective clothing from UV rays by applying sunscreen frequently, using protective clothing when outdoors and minimizing sun exposure as much as possible.
- Lifestyle Management: Balancing stress management, exercise routines and diet is essential to overall well-being and may reduce the frequency of disease flare-ups.
- Kidney Involvement: For patients diagnosed with Lupus Nephritis (kidney involvement), treatment may include medications and close monitoring by a nephrologist.
- Routine Monitoring: People living with SLE need regular follow-up with a rheumatologist or healthcare provider in order to monitor disease activity, manage medications and address any emerging symptoms or complications.
Oral Health Impact: Lichen Planus vs. Lupus Erythematosus
Lichen Planus:
- Oral Involvement: Lichen Planus is known to affect the oral cavity, leading to Oral Lichen Planus (OLP). OLP manifests itself with white lacy patches, painful sores or ulcers on cheeks, tongue, gums and other oral mucous membranes inflicting white lacy patches, sores or ulcers on them that appear white in color with lacy edges lining each patch typically manifesting themselves on cheeks tongue gums and other mucous membranes affected.
- Symptoms: OLP can cause considerable discomfort, from pain and burning sensations to sensitivities to spicy or acidic foods, in severe cases compromising one’s ability to eat, speak or maintain proper oral hygiene.
- Diagnosis and Treatment of Orofacial Lymphoma: Diagnosis typically includes clinical examination and, in certain instances, biopsies. Treatment options for OLP typically include corticosteroids, immunosuppressants, oral rinses or gels containing medications to ease symptoms and decrease inflammation, regular dental check-ups are crucial in monitoring and managing oral health.
Lupus Erythematosus (SLE):
- Oral Manifestations of Lupus: Lupus can also have an adverse impact on the oral cavity, manifesting with various manifestations in its mouth such as ulcers (canker sores), lesions and redness in its oral tissues symptoms which collectively refer to as Lupus Oral Ulcers (LOU).
- Symptoms: LOU can cause pain and discomfort, making eating, speaking and maintaining oral hygiene challenging. The presence of LOU could signal disease activity or an inflammation flare-up.
- Diagnosis and Management: Lupus can be diagnosed through clinical examination, which may provide an indicator of its activity. Medication to manage systemic lupus activity may also help, with oral symptoms often linked to overall disease activity; patients may use topical treatments or oral rinses for extra comfort if needed.
Comparison:
- Lichen Planus and Lupus Erythematosus can both have detrimental effects on oral health, leading to pain, discomfort, and functional limitations.
- Lichen Planus typically affects the oral mucosa with characteristic white lacy patches or ulcers while Lupus Erythematosus may result in mouth ulcers and lesions in some instances.
- Management of oral symptoms in both conditions involves treating both their source (the disease itself) and providing symptomatic relief, potentially using topical treatments or medications as needed.
- Regular dental check-ups and collaboration between dermatologists or rheumatologists and dentists is vital in order to monitor and manage oral health in individuals living with dermatologic or rheumatic diseases.
Difference Between Lichen Planus and Lupus Erythematosus
Lichen Planus is an autoimmune condition that mostly affects mucous membranes and the skin however, lupus-erythematosus is an autoimmune condition that predominantly is a problem for joints, skin kidneys, blood vessels as well as the brain heart, and the lungs. So, that’s the main distinction between lichen planus and lupus, a condition that is characterized by a rash of blood.
Lupus planus may be brought on by hepatitis C disease, the flu vaccine, specific pigments, metals, chemical compounds, and pain killers such as naproxen and ibuprofen, as well as some heart-related medications as well as high blood pressure as well as arthritis.
It is possible that lupus may be caused by sun as well as infections and medication (anti-seizure medication as well as antibiotics).
Here is a comparison chart between Lichen Planus and Lupus Erythematosus:
| Feature | Lichen Planus | Lupus Erythematosus (SLE) |
|---|---|---|
| Nature | Inflammatory skin/mucous membrane condition | Autoimmune systemic disease |
| Etiology | Unknown, possibly autoimmune | Autoimmune (genetic and environmental factors) |
| Common Symptoms | Itchy, flat-topped purplish or reddish-brown papules, lace-like pattern | Fatigue, joint pain, skin rashes (butterfly rash), photosensitivity, organ involvement |
| Mucous Membrane Involvement | Frequently affects mucous membranes (Oral Lichen Planus) | Can affect various organs, including mucous membranes |
| Diagnosis | Clinical examination, biopsy for confirmation | Combination of clinical criteria, blood tests (e.g., ANA), and sometimes biopsies |
| Types | Cutaneous, Oral, Genital, and more | Systemic Lupus Erythematosus (SLE), Cutaneous Lupus Erythematosus (CLE), Discoid Lupus Erythematosus (DLE), and others |
| Treatment | Topical corticosteroids, immunosuppressants, antihistamines | Immunosuppressive medications, anti-inflammatories, and symptom-specific treatments |
| Prognosis | Generally not life-threatening; varies by severity | Chronic condition with a range of outcomes, potentially life-threatening in severe cases |
| Disease Severity | Typically localized to skin and mucous membranes | Can be systemic, affecting multiple organs and systems |
| Onset | Can occur at any age, most common in middle-aged adults | Typically begins in young adulthood, more common in women |
| Long-term Management | May require long-term management but often less intensive | Requires ongoing medical care, monitoring, and potential lifestyle adjustments |
| Differential Diagnosis | Often based on clinical appearance, may resemble other skin conditions | Requires differentiation from various autoimmune and inflammatory diseases |
Preventive Strategies for Health in Lichen Planus and Lupus Erythematosus
Preventive Strategies for Health in Lichen Planus:
- Avoid Triggers: Be mindful to identify and eliminate potential triggers that could aggravate Lichen Planus symptoms, such as specific medications, dental products or stressors.
- Oral Hygiene: For optimal oral hygiene in Oral Lichen Planus (OLP), maintain proper dental practices such as regular brushing, flossing and using non-irritating toothpaste. These measures will reduce your risk of oral complications.
- Regular Dental Check-Ups: Visit a dentist or oral health specialist regularly for exams that can detect early signs of OLP and offer guidance for managing oral health. These exams may help detect early warning signals.
- Gentle Dental Care: Before seeking any dental treatments or cleanings, inform your dentist of your condition so they can use gentle techniques and non-irritating products to minimize trauma to oral tissues.
- Oral Rinses: Depending on the severity and type of OLP, healthcare providers may prescribe medicated oral rinses or gels to alleviate discomfort and inflammation. Carefully follow their instructions.
- Stress Reduction: Stress has long been recognized as a trigger of Lichen Planus flares. Engage in stress-reducing techniques such as mindfulness meditation or yoga in order to effectively combat this potential trigger and manage your stress effectively.
Preventive Strategies for Lupus Erythematosus (LE), particularly Systemic Lupus Erythematosus (SLE):
- Medication Adherence: Be sure to adhere to your treatment plan recommended by your rheumatologist or healthcare provider in order to properly manage lupus flare-ups and decrease flares.
- Sun Protection: Avoid UV radiation as long exposure can worsen skin symptoms of Lupus flare-ups. Use broad spectrum sunscreen, wear protective clothing and limit sun exposure as much as possible.
- Lifestyle Management: Lead an active and healthy lifestyle, including exercising regularly, eating nutritiously, limiting smoking and excessive alcohol consumption and not smoking, to support overall well-being and immune health. These practices will contribute to overall well-being and immunity health.
- Stress Reduction: Stress reduction is of great importance to those living with lupus as stress can worsen symptoms. Try engaging in stress relief techniques such as relaxation exercises, hobbies or support groups to alleviate any unnecessary tension or anxiety.
- Regular Checkups: Regular appointments with your rheumatologist or healthcare team should be scheduled to monitor disease activity and adjust treatments as necessary. Regular assessments allow doctors to evaluate disease progression while adapting treatments accordingly.
- Vaccinations: Stay up-to-date with vaccinations and seek the advice of your healthcare provider when considering new vaccines as some may not be appropriate for people with compromised immune systems.
- Collaboration Care: Maintain open communications among your rheumatologist, dermatologist and dentist for optimal treatment of systemic and oral health needs. By working together as healthcare providers you may better meet both needs.
- Oral Health: Pay particular attention to oral health by adhering to a regular oral hygiene routine and attending dental check-ups, while promptly responding to any oral symptoms that could be indicative of lupus activity.
Summary
Lichen Planus, or Lichens Planus, is a chronic inflammatory skin and mucosal condition characterized by itchy flat-topped lesions and papules with mucous membrane involvement. Although its cause remains unknown, its primary contributor may involve autoimmunity; diagnosis relies on clinical exams and biopsies when necessary for accurate diagnoses.
While topical corticosteroids and immunosuppressants are frequently prescribed to manage its symptoms; Lichen Planus usually remains localized and life-threatening conditions compared to more serious conditions like Lupus or MS.
Lupus Erythematosus encompasses systemic and cutaneous forms of Lupus Erythematosus (SLE). SLE is a systemic autoimmune disease with symptoms including skin rashes, joint pain, internal organ issues and other organ-specific issues.
Diagnosis typically requires criteria and lab tests; management includes immunosuppressants or treatment targeted to individual symptoms with lifelong conditions of various severity being considered. Lupus can affect people of any age at any point during life.