Introduction of Immediate and Delayed Hypersensitivity
Immediate and Delayed Hypersensitivity reactions involve immune responses triggered by sensitization and subsequent exposure to specific antigens.
Immediate hypersensitivity (IH) is an acute immune reaction caused by IgE antibodies upon exposure to allergens, manifested as allergies, asthma and anaphylaxis symptoms. Mast cells and basophils release histamines which result in rapid responses.
Delay hypersensitivity refers to T cell-mediated reactions occurring hours or days post-exposure, when CD4+ and CD8+ T cells respond to antigens by engaging their CD8 receptors, leading to macrophage activation and activating cytotoxic T cells Examples include contact dermatitis and tuberculin reactions.
Differentiating between immediate hypersensitivity and delayed hypersensitivity is crucial for accurate diagnosis and treatment approaches ranging from antihistamines and epinephrine for immediate responses, while corticosteroids and immunosuppressive agents can assist when treating delayed hypersensitivity symptoms.
What is Immediate Hypersensitivity
Immediate hypersensitivity (also referred to as Type I hypersensitivity) is an extreme and rapid immune reaction triggered by certain allergens that leads to mast cells and basophils producing specific antibodies called immunoglobulin E (IgE), binding quickly with them and producing inflammation as soon as they enter your system.
It involves producing specific immunoglobulin E antibodies called immunoglobulin E that produce IgE molecules to bind with mast cells and basophils which in turn bind directly with these two white blood cell types upon contact, leading to immediate hypersensitivity reactions caused by allergen exposure. IgE molecules produced to create this rapid immune reaction caused by exposure.
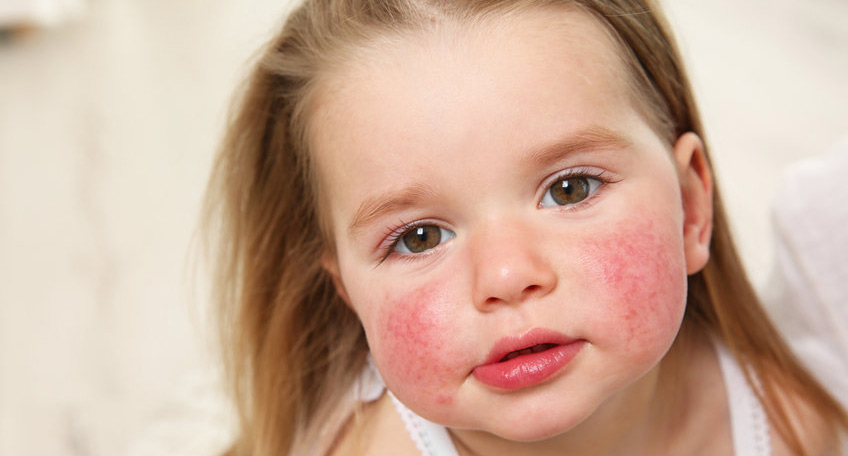
This immediate hypersensitivity reaction involves producing specific IgE antibodies to attach directly with mast cells and basophils which then react by binding with mast cells or basophils white blood cell types in response.
Subsequent exposures of an allergen will bind with IgE antibodies attached to mast cells and basophils, activating their activation and release of chemical mediators such as histamine which then cause dilation of blood vessels, increased permeability of vessel walls.
Smooth muscle contraction, dilation, swelling, itching, swelling hives difficulty breathing or potentially life-threatening anaphylaxis symptoms resulting in immediate hypersensitivity symptoms including itching swelling hives difficulty breathing even life-threatening anaphylaxis symptoms in immediate hypersensitivity patients.
Examples of immediate hypersensitivity reactions include allergic rhinitis (hay fever), asthma, and food allergies with symptoms appearing within minutes after allergen exposure and often within minutes after diagnosis with methods like skin prick tests and measurement of serum IgE levels. Treatment often entails avoiding allergens as much as possible or, in severe cases, administering medications like antihistamines and epinephrine to swiftly counteract allergic responses.
What is Delayed Hypersensitivity?
Delayed hypersensitivity (also referred to as Type IV hypersensitivity) is an immune response that typically arises hours to days post exposure to allergens, pathogens, or self-antigens that causes immediate hypersensitivity via antibodies such as IgE. By contrast, delayed hypersensitivity relies more heavily upon T cells (specifically CD4+ and CD8+ T cells) rather than IgE antibodies to trigger its response.
Once exposed to antigen, sensitized CD4+ T cells become activated and initiate a cascade of immune reactions in response. These activated T cells release various cytokines which attract macrophages and cytotoxic CD8+ T cells from other immune cells to the site of exposure; both groups contribute towards tissue damage and inflammation within affected areas.
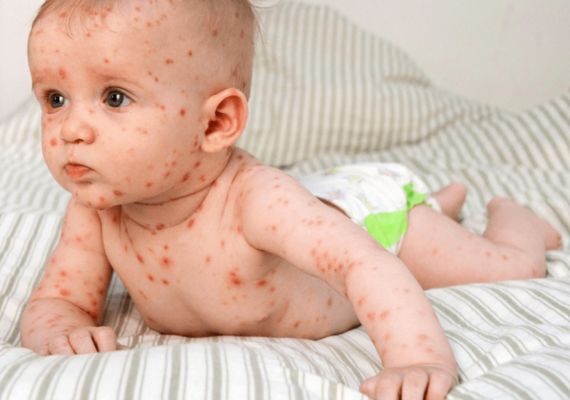
Common forms of delayed hypersensitivity reactions include contact dermatitis from poison ivy exposure, tuberculin skin tests used to diagnose tuberculosis and certain autoimmune diseases like type 1 diabetes and multiple sclerosis. Characteristically delayed hypersensitivity reactions feature gradually developing symptoms with T cells being involved.
Patch tests or tuberculosis skin tests may be performed as diagnostic tools while treatment options often include treating its root cause while managing inflammation as well as taking immunosuppressant drugs to block your immune response.
Importance of understanding the differences between immediate and delayed
Understanding the differences between immediate and delayed hypersensitivity reactions is of vital significance in clinical settings as well as research settings, with significant ramifications for patient management, accurate diagnosis, and the development of targeted therapies.
- Accurate Diagnosis and Treatment: Making an accurate diagnosis and effective treatment decisions requires distinguishing between the two forms of hypersensitivity reactions. Misidentifying them could result in ineffective or harmful therapies; for instance giving antihistamines to someone with delayed hypersensitivity might not bring desired results.
- Clinical Management: Understanding the symptoms associated with immediate and delayed hypersensitivity allows clinicians to select appropriate interventions. Immediate hypersensitivity reactions, like anaphylaxis, require prompt administration of epinephrine and antihistamines; delayed hypersensitivity might require anti-inflammatory agents like corticosteroids in order to effectively address immune-mediated tissue damage.
- Patient Education: By teaching patients the nature of their hypersensitivity reactions, we enable them to recognize early symptoms and take effective actions to combat it. With such knowledge at their disposal, individuals who suffer from allergies or sensitivities to allergens can avoid triggers while seeking timely medical help for treatment and avoid long-term problems as a result.
- Research and Therapeutic Development: It is vital that researchers gain an in-depth knowledge of both types of hypersensitivity reactions in order to design effective therapies. Researchers may target specific immune pathways with drugs designed to modulate immune reactions for more targeted, safer treatments.
- Public Health and Prevention: Understanding the difference between immediate and delayed hypersensitivity reactions can aid public health efforts by helping identify outbreaks involving these reactions, such as tuberculosis or allergic contact dermatitis.
- Immunization and Vaccine Development: Understanding hypersensitivity reactions is integral to vaccine design strategies; vaccines should aim at inducing protective immune responses without inciting harmful hypersensitivity reactions.
Causes and Symptoms of Immediate and Delayed Hypersensitivity Reaction
What causes and signs of an immediate hypersensitivity reaction:
Hypersensitivity symptoms that are immediate in nature are caused by the exposure of allergens, which trigger a swift immune response that is mediated by IgE antibodies.
Common causes include:
- Allergens Pollen, for example, dust mites, pollen, animal vermin, insects as well as certain food items.
The signs of an immediate reaction to hypersensitivity are:
- Skin The symptoms include hives (urticaria) and redness, itching, and swelling.
- Respiratory symptoms: Runny nose, sneezing, and nasal congestion. Also wheezing, coughing, and shortness of breath.
- Gastrointestinal The vomiting, nausea abdominal pain, diarrhea.
- Anaphylaxis Inspiring symptoms such as throat swelling trouble breathing, a sudden decrease in blood pressure and the loss of consciousness.
The causes and symptoms of delayed hypersensitivity reaction:
Delayed hypersensitivity reactions can be characterized as T-cell-mediated reactions that occur within hours or days following contact with antigens.
The most common causes are:
- Infections Bacterial, viral and fungal diseases.
- Allergens Certain delayed reactions may trigger through allergens, too.
The symptoms caused by delayed reactions to hypersensitivity are:
- Skin: Erythema (redness) as well as Inflammation (hardening) and an increase in the size of the skin at the exposure.
- Tissue Injuries: Inflammation, tissue destruction, and the formation of lesions.
- Symbiotic: In cases of chronic delayed hypersensitivity, symptoms such as fever, malaise and fatigue could be present.
Comparison between Immediate and Delayed Hypersensitivity
Here’s a simplified comparison chart between Immediate and Delayed Hypersensitivity:
| Aspect | Immediate Hypersensitivity | Delayed Hypersensitivity |
|---|---|---|
| Onset | Rapid (within minutes) | Delayed (hours to days) |
| Immune Mediators | IgE antibodies, mast cells, basophils | CD4+ and CD8+ T cells, macrophages |
| Activation Mechanism | Cross-linking of IgE, mast cell degranulation | Activation of sensitized T cells |
| Clinical Manifestations | Allergies, asthma, anaphylaxis | Contact dermatitis, tuberculin reaction |
| Inflammation Mechanism | Histamine release, vascular dilation | Cytokine release, immune cell infiltration |
| Diagnostic Methods | Skin prick tests, serum IgE levels | Patch tests, tuberculin skin tests |
| Treatment | Antihistamines, epinephrine (anaphylaxis) | Corticosteroids, immunosuppressive agents |
| Time Frame | Immediate response | Delayed response |
| Examples | Allergic rhinitis, food allergies | Poison ivy reaction, tuberculosis |
| Mechanism of Action | Antigen-IgE-mast cell interaction | Antigen-T cell interaction |
| Tissue Damage | Limited tissue damage | Substantial tissue damage |
What are the Similarities Between Immediate and Delayed Hypersensitivity?
Here are a few similarities between both types of hypersensitivity reactions:
- Immune System Components: Immediate and delayed hypersensitivity reactions utilize various components of the immune system – IgE antibodies and mast cells are typically involved, while delayed reactions might involve CD4+ or CD8+ T cells which often trigger delayed reactions.
- Inflammation: Both types of reactions result in inflammation at the site of exposure. With immediate hypersensitivity, histamine release causes rapid vasodilation and increased vascular permeability leading to redness, swelling and itching; with delayed hypersensitivity cytokines attract immune cells leading to delayed inflammation responses.
- Clinical Manifestations: Both types of reactions may lead to skin manifestations; immediate hypersensitivity usually manifests itself with hives, itching and redness while delayed hypersensitivity typically presents itself through skin rashes, redness or blisters.
- Diagnostic Testing: Hypersensitivity reactions can be detected using specific tests for both immediate and delayed reactions, with skin tests often providing the best assessment; skin prick tests or patch tests may also be administered directly or delayed to measure reactions accordingly.
- Immune Memory: Reactions can provoke immune memory responses upon exposures that result in faster and more intense responses when exposed again – such as allergens or antigens that trigger them a second time around, creating faster reactions upon repeated encounters with them.
- Prevention: Avoidance of allergens or antigens is often recommended as an effective measure against both immediate and delayed hypersensitivity reactions, with patients often given advice to identify and limit exposure to triggers.
- Treatment Approach: Although treatment strategies differ depending on the cause and mechanism of hypersensitivity reactions, both focus on managing inflammation and symptoms. Corticosteroids contain anti-inflammatory properties which make them highly effective against both immediate and delayed hypersensitivity reactions.
- Clinical Importance: Understanding the differences and similarities between two forms of hypersensitivity reactions is paramount in order to provide accurate diagnoses, effective therapies and patient education. Differentiation helps healthcare providers provide appropriate interventions.
Factors Influencing Hypersensitivity Reactions
Hypersensitivity reactions, both immediate and delayed, are determined by various combinations of genetic, environmental, immunological, and historical exposure factors. Gene predisposition can play an integral part in hypersensitivity reactions; certain people inherit genes that make them more prone to them; variations related to immunity such as IgE receptors or T cell receptors can increase risk significantly and influence severity.
Environmental factors also have an effect, with repeated exposure to allergens or antigens leading to sensitization and altering an individual’s immune response. Environmental pollutants and allergen exposure increase the likelihood of hypersensitive reactions among atopic individuals, potentially increasing hypersensitive reactions significantly.
Immunological factors encompass complex interactions among immune cells, antibodies, and cytokines that come together in complex patterns to form pro-inflammatory and regulatory immune responses that determine both the type and intensity of hypersensitivity reactions.
An allergen or antigen’s prior exposure also influences its immune response, potentially sensitizing your system to it and producing specific antibodies or memory T cells that respond with greater intensity on future exposures. This initial exposure could trigger sensitization; subsequent ones might trigger further upsurges in responses.
Immune system health is of critical importance. Any deficiencies or dysregulation that disrupt the normal response to antigens could trigger extreme or inappropriate hypersensitivity responses that cause exaggerated or inappropriate hypersensitivity reactions.
Understanding this complex interaction of genetic, environmental, immunological, and previous exposure factors is vital in comprehending why some individuals may be more prone to hypersensitivity reactions than others and creating effective prevention and treatment plans for them.
What is the most effective treatment for Immediate and Delayed Hypersensitivity?
Treatment strategies for immediate and delayed hypersensitivity reactions depend on their causes and clinical manifestation.
Here’s an overview:
Immediate Hypersensitivity Reactions:
The primary goal in treating immediate hypersensitivity reactions is to quickly address symptoms and stop the progression to more serious reactions such as anaphylaxis.
Interventions for treating immediate hypersensitivity reactions typically include:
- Antihistamines: These antihistamines block histamine release to provide temporary relief of itching, hives and sneezing related to allergic reactions.
- Epinephrine: Epinephrine (adrenaline) should only be administered in severe instances of immediate hypersensitivity or anaphylaxis to quickly counteract symptoms by constricting blood vessels, opening airways and stabilizing blood pressure.
- Bronchodilators: For immediate hypersensitivity reactions involving the respiratory system, inhalers such as bronchodilators may help open airways and improve breathing in conditions like allergic asthma.
Delayed Hypersensitivity Reactions:
Delayed hypersensitivity reactions involve different immune mechanisms and often require anti-inflammatory strategies in order to manage tissue damage and inflammation:
- Corticosteroids: Corticosteroids are powerful anti-inflammatory medicines commonly prescribed to suppress immune reactions in delayed hypersensitivity reactions, helping reduce inflammation, alleviate symptoms and protect tissue damage from further happening.
- Immunosuppressive Agents: For patients experiencing serious or persistent delayed hypersensitivity reactions, immunosuppressant drugs may be prescribed in order to suppress immune reactions and limit tissue damage.
- Topical Therapies: For delayed hypersensitivity reactions on the skin such as contact dermatitis, topical corticosteroid creams or ointments may provide direct inflammation control while attenuating itching symptoms.
- Avoidance: In both immediate and delayed hypersensitivity reactions, avoiding allergens or antigens which trigger reactions is key in order to minimize or avoid reactions altogether.
Summary
Hypersensitivity reactions are immune responses that may either be immediate or delayed in their onset. IgE antibodies cause immediate reactions such as allergies and anaphylaxis; delayed hypersensitivity involves T cells which manifest later, such as contact dermatitis.
Both types cause inflammation in skin manifestations as well as diagnostic methods used for diagnosis; both types require accurate diagnoses to provide effective care plans; immediate reactions require antihistamines while delayed ones often need corticosteroids for management – understanding their differences is vital in order to provide effective care strategies.

